|
9/12/2023 0 Comments Pathological hypertrophy heart
Normal response to aerobic conditioning leads to enlargement of the myocytes with preserved architecture and corresponding expansion of the capillary beds. The heart possesses a unique three-dimensional architecture in which helically arranged myocardial fibres are embedded in a dense fibrous matrix. The cardiomyocytes stop increasing in number soon after birth but retain marked plasticity which enables them to adapt to a variety of environmental stimuli with increase in size, or contraction. Physiologic versus pathologic hypertrophy 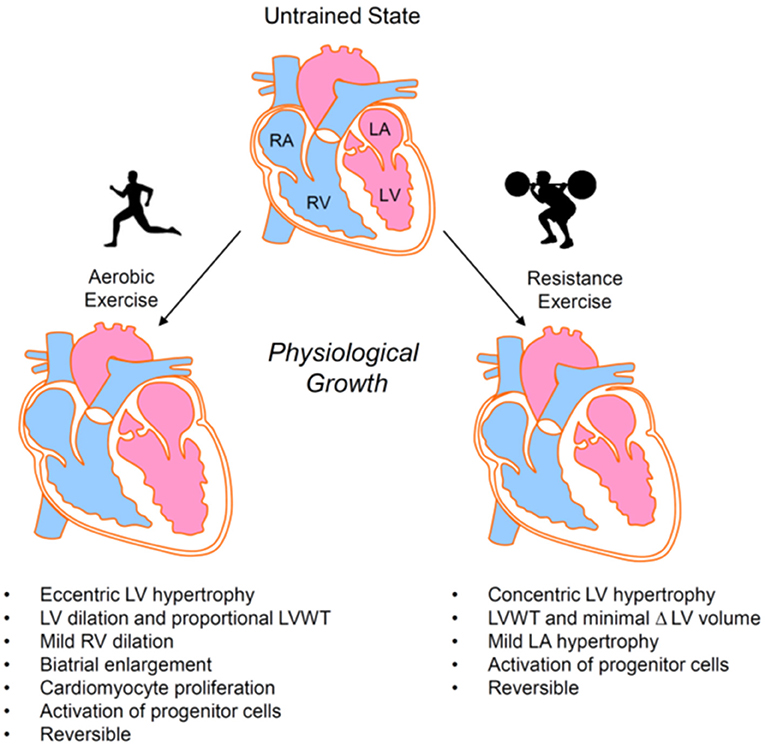
Hence, the impairment of LV function concomitant with various deleterious factors influencing peripheral flow and tissue metabolism (cocaine, anabolics, amphetamine, exercise-induced hyperthermia), may not only affect the maximal exercise performance in athletes, but also contribute to serious cardiovascular complications during or after exercise. In view of these inconsistencies, a new, “evolutionary-biological” circulation model has recently been proposed in which the flow of blood is regulated by the metabolic demands of the tissues and the heart acts as an impedance pump which maintains pressure by rhythmically interrupting the flow. However, the effectiveness of muscle pump in dynamic exercise has also been questioned. The source of “missing” blood volume - a long-standing dispute among exercise physiologists - is supposedly supplied by a “muscle pump”, a mechanism by which the blood is returned to the heart by the contracting muscles. Because of these physical limitations, the maximally performing exercising heart can account for about half of the volume throughput measured in high-performance athletes, known to be in the region of over 30 L/min. Due to greatly increased heart rate, the improved diastolic filling is offset by a progressively shortened diastolic filling time. Beta-adrenergic stimulation and improved diastolic compliance account for increased cardiac contractility and filling of up to 60% (Frank-Starling mechanism). min-1, or 100-fold above the basal values ! In untrained athletes, the mean stroke volume (SV) increases by one third before reaching a plateau, whereas in highly trained athletes the SV continues to rise progressively to the point of maximal exercise.This adaptive physiology is needed to meet the greatly increased demand for oxygen by a large mass of muscles which is perfused up to a 2.5 L Exercise haemodynamicsĪ normal response to incremental dynamic exercise is a doubling in heart rate (HR), a threefold or fourfold increase in cardiac output (CO), a moderate increase in mean arterial pressure (MAP) and markedly decreased total peripheral resistance. Heart failure in athletes – pathophysiology, inducing factors and clinical consequences 1. Hence, a detailed screening of athletes with high risk of HF by means of advanced diagnostic techniques is called for. A recent registry analysis demonstrates that myocarditis can be a dominant cause of sudden cardiac death in athletes under 35. The inflammatory process of the myocardium can result in a fulminant HF in athletes engaged in intensive exercise, overtraining, doping, or drug abuse. The latter may run an asymptomatic course and present with normal resting electrocardiography in up to 32% of those affected. Dilated cardiomyopathy is the main cause of HF in athletes, while acute myocarditis is the most frequent cause of acquired dilated cardiomyopathy in young athletes. In addition, HF of various other aetiologies can also contribute to cardiovascular fatalities in this population. Equipped with an improved diagnostic and treatment armamentarium, and faced with a growing number of “at risk” participants, sports cardiologists will be increasingly faced with the dilemma of qualifying this population for exercise.Īccording to the well-known mortality classifications, hypertrophic cardiomyopathy is the leading cause of sudden cardiac death in athletes. Moreover, a greater number of patients with a history of cancer treated with cardiotoxic therapy seek participation in sports. The risk of unrecognised symptomatic or asymptomatic left ventricle (LV) remodelling with subsequent heart failure (HF) in athletes increases with age. In recreational sports, the incidence of sudden cardiac death and cardiovascular comorbidities is higher than expected and may even increase as more and older individuals participate in organised sports. A growing interest in sports activities raises concerns regarding the safety of exercise in athletes with various cardiovascular anomalies.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
